Making Medicaid Work Better in Minnesota
Our health insurers lead the nation in the way they help Minnesotans with Medicaid get care.The Numbers Tell the Story
1 in 5 Minnesotans
receive their medical insurance through either MinnesotaCare or Medicaid.
1 in 4 Minnesota Kids
receive their medical insurance through Medicaid.
1 in 2 Minnesota Nursing Home Residents & People with Disabilities
receive their medical insurance through Medicaid
You Might Be Surprised to Learn That …
- Medicaid isn’t a federal program; it’s a federal and state program. In Minnesota, the federal government pays about 57% of the costs, while the State of Minnesota pays the remaining 43%.
- Minnesotans receive their Medicaid coverage through our nonprofit health insurance companies, and those companies provide access to dozens of additional services to improve their health and well-being.
Top 10 Reasons Why Minnesota's Medicaid Is a National Model
Minnesota’s nonprofit health insurance companies are nationally recognized for their efforts to improve the well-being of Minnesotans who get their health insurance through Medicaid. Here's why.1
We help Minnesota seniors maintain excellent communication with clinics and social service providers, and that helps them manage their diabetes and other medical conditions.
2
We’ve increased the number of Minnesota kids who get immunizations and have their blood tested for lead—especially in the Hmong community, where child visit rates are usually low.
3
We help Minnesotans with asthma better manage their condition so they can avoid going to the hospital or emergency room.
4
We increase the number of Minnesota kids who receive health checkups at home, and working with faith-based organizations to overcome language and cultural barriers to make sure more kids get their regular health screenings.
5
We motivate Minnesota teens to attend regular doctor visits.
6
We make it easier Minnesotans to get dental care.
7
We encourage Minnesotans to take advantage of childbirth education, healthy lifestyle education, cancer screenings, prenatal care and other resources that help prevent disease.
8
Helped doctors and others who provide care for people who have addictions to pain medications. The help included special information on how to help people manage pain without opioids—
the medications that are highly addicting.
People who care for Minnesotans who live with addiction as well as depression or other mental illness got extra training.
- Here is the information shared with doctors and others who provide care
- Here are other ways to manage pain
- Presentations for pharmacists, alternatives to opioids, additional help for people with mental illnesses
9
We help communities throughout the state to take on social issues that have a big impact on a person’s health. Sometimes that help includes getting healthy food, finding a place to live or finishing school.
10
We work to close Minnesota’s high racial and ethnic disparities by supporting improvements not only in health, but also in education, employment, transportation, housing, income and justice.
Get Medicaid or MinnesotaCare
- Here is where you sign up. The sign up system will put you in the right kind of insurance. It depends on how old you are, where you live and how much money you make each month.
- Here you can find a map of counties across Minnesota and what companies can help people get the care they need.
- Here you can find information on each company, such as what state reviews have to say about the work, how satisfied current enrollees are with the care they get and more.
For people over 65 or living with disabilities
Minnesota’s public insurance options that combine Medicare and Medicaid are the envy of many health policy experts across the country.
One kind of insurance, Minnesota Senior Health Options, is for people 65 and older who qualify for both Medicare and Medicaid.
Another kind of insurance, Special Needs BasicCare, is for people who live with disabilities. Pages two and three of this document outline the difference between selecting to get care with the help of a health insurer versus signing up directly with the state.
Here is information on how health insurers can help you stay in your home.
What Others Have to Say
Writers at HealthAffairs say that Minnesota’s approach is a model for the rest of the country. A recent evaluation, they said, of Minnesota Senior Health Options program, showed a 48 percent reduction in inpatient hospitalizations and a 26 percent reduction in the total number of hospital stays for patients who were hospitalized during the year. The researchers at Long Term Services and Supports rank Minnesota at #2 in the country on its work so far to improve services for older adults and people with physical disabilities, and their family care partners. Minnesota’s scores are worse than the national average on percent of people living in nursing homes who have low needs for care, and the percent of people with home health care who end up needing to be hospitalized.
Minnesota earned recognition for its work to reduce the chances of someone needed to be in a care facilities a long time after they were hospitalized.
Contact Your Health Insurer
Quality
Minnesota’s health insurers helped launch MN Community Measurement more than 10 years ago. Since then, the care Minnesotans get continually improves. This report shows the different outcomes by the type of insurance people have. This report shows results when looking at information based on race, Hispanic ethnicity, language and what country people are from.
State Partnerships
Helping all Minnesotans get the care they need
Health insurers were brought in by the state more than 30 years ago to help manage overall expenses and ensure people who get help paying for care through Medicaid could find a doctor. Strict rules and careful oversight ensure that the companies are providing the best possible care to Minnesotans—and that they are being responsible stewards of tax dollars in the process. These insurers serve people across Minnesota, not shareholders on Wall Street.
Commited and accountable to Minnesotans
The state hires health insurers to provide health insurance and care coordination to people with state insurance. Minnesota does this because lawmakers understand health insurers have unique capabilities—financial structures, medical knowledge, administrative knowhow and relationships with doctors and others who provide care—that enable people to get the best possible care, at the lowest possible cost to taxpayers. Information about how the insurers are doing providing these services and how money is spent is available on the managed care reporting page of the DHS website.
Personalized care
The state’s health care programs serve Minnesota families and children who do not have much money, seniors who need extra help beyond Medicare, and people with disabilities. As a result of the insurers’ partnership with Minnesota, people who get care through the state can see same doctors as people with insurance through employers. Gone are the days when a person with Medicaid insurance can’t receive care near his/her home. Today, people can get care through telemedicine, online convenience care, at retail outlets and of course in their hometown clinic. Nurses through the health insurers are available 7 days a week, 24 hours a day to help people get the care they need.
When you’re sick or have been recently diagnosed with an ongoing illness, getting well can be a full-time job. Our insurers help Minnesotans understand their condition and learn what it takes to get better. In addition, people who need a lot of care get help figuring it out with assistance from people whose job it is to get necessary appointments, coordinate the care, etc.
Over the years, insures have worked with the state to create specialized care for Minnesotans who elderly or live with disabilities, combining two programs—Medicare and Medicaid—into one package. This means people get rides to clinic appointments, help at home, interpreter services and other services they didn’t get before.
Insurers also study data to help identify if people would like help they aren’t getting. By spotting potential concerns, insures can help connect people with health and wellness programs, or other services. The analysis of data also allows insures remind people to get necessary checkups and encourage healthy activities.
Commited and accountable to Minnesotans
The state hires insurers to provide health insurance and care coordination to people with state insurance. Minnesota does this because lawmakers understand health insurers have unique capabilities—financial structures, medical knowledge, administrative knowhow and relationships with doctors and others who provide care—that enable people to get the best possible care, at the lowest possible cost to taxpayers. Information about how the insurers are doing providing these services and how money is spent is available on the managed care reporting page of the DHS website.
A rich history
To find out more about the history of managed care in Minnesota, read Minnesota’s journey toward universal coverage
Responsible stewards of tax dollars
The state decides what services and treatments are covered, who is eligible and then signs people up. It pays insurers a set amount per person for all covered services—and nothing more. Insurers take it from there. They use expertise in IT, data monitoring, working with providers and more to get people the care they need. Insurers pay all bills. If payments from the state don’t cover the medical bills, like in 2016, the insurer still pays. Shifting financial responsibility to the insurers gives the state a stable and predictable budget.
Since in the past five years, the health insurers had less than 0.5% of the money they received from the state at the end of the year. That’s 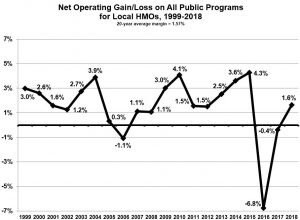 tight, but local insuers are here to stay, in good times and bad. In the past 20 years, the average margin after all the bills are paid is 1.6%, so seen in the graph at right.
tight, but local insuers are here to stay, in good times and bad. In the past 20 years, the average margin after all the bills are paid is 1.6%, so seen in the graph at right.
